London surgeon performs remote prostatectomy in Gibraltar
Toumai robotic system runs over fibre with 5G backup, liability question moves from scalpel to network
Images
 Paul Buxton and partner Lucia. After his diagnosis, he had expected to join an NHS waiting list and travel to England because of the operation’s complex nature. Photograph: Paul Buxton/PA
theguardian.com
Paul Buxton and partner Lucia. After his diagnosis, he had expected to join an NHS waiting list and travel to England because of the operation’s complex nature. Photograph: Paul Buxton/PA
theguardian.com
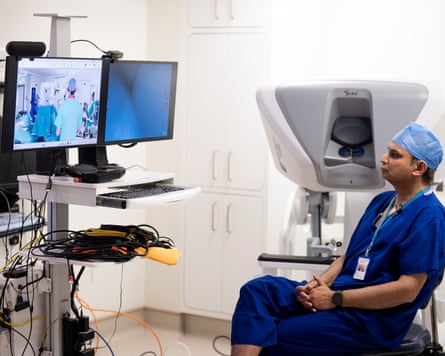 Prof Prokar Dasgupta preparing to perform the remote telesurgery operation on 4 March. Photograph: Aaron Chown/PA
theguardian.com
Prof Prokar Dasgupta preparing to perform the remote telesurgery operation on 4 March. Photograph: Aaron Chown/PA
theguardian.com
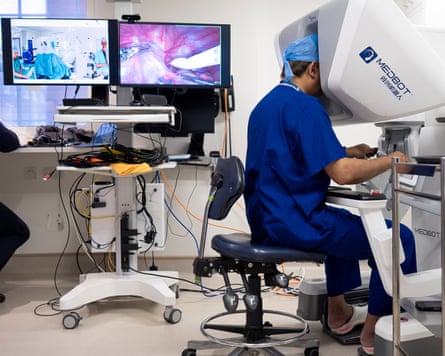 The operation, using the Toumai Robotic System, begins. Photograph: Aaron Chown/PA
theguardian.com
The operation, using the Toumai Robotic System, begins. Photograph: Aaron Chown/PA
theguardian.com
A surgeon in London has performed a prostatectomy on a patient in Gibraltar using a robot in a theatre 1,500 miles away, according to The Guardian. The operation at St Bernard’s Hospital used a four-armed Toumai robotic system controlled by Prof Prokar Dasgupta from a console in Harley Street, with a reported time delay of 0.06 seconds.
The system was linked via fibre optics with a backup 5G connection, and a local team in Gibraltar stood ready to take over if the connection dropped. The patient, 62-year-old Paul Buxton, said he expected to join an NHS waiting list and travel to England for complex surgery but instead underwent the procedure locally, describing it as a “no-brainer” given the alternative of weeks away from home.
The clinical milestone is easy to describe; the operational one is harder. Remote robotic surgery shifts the centre of gravity from the operating room to the communications chain: routing, redundancy, latency and failure modes become part of the procedure. That in turn raises the question that health systems and insurers tend to postpone until something goes wrong: who is responsible when the harm is caused not by a scalpel slip but by a software fault, packet loss, or a telecom outage.
In a conventional operation, liability tends to sit with the surgeon and the hospital, with device makers facing product claims when a defect can be shown. In a cross-border telesurgery setup, the list of actors expands: the surgeon’s employer, the treating hospital, the robot manufacturer, the technology services provider that integrates the system, and the network operator carrying the connection. Each has an incentive to define the failure as someone else’s domain—clinical judgement, device performance, IT integration, or “force majeure” in the network.
The Guardian notes that a team was present on site to take over if the link failed, a practical hedge that also functions as a legal one: it provides a human backstop, but it also makes it easier to argue that the remote link is an assistive tool rather than the sole critical path. The more common remote surgery becomes, the harder it will be to staff duplicate teams, and the more pressure will fall on contracts and insurance to decide in advance which failures are covered and at what price.
Regulators, meanwhile, will be pulled in two directions. Remote surgery promises access to specialist care without travel, which is politically attractive for peripheral regions and small jurisdictions. But every additional approval layer—licensing across borders, mandated network standards, reporting requirements—creates a new point of delay that patients notice long before they notice hypothetical cyber risks.
Buxton’s operation was completed with a measured delay of 60 milliseconds and a standby team in the room. The next dispute will not be about whether the robot can cut—it will be about who pays when the connection does not hold.
