London measles outbreak exposes school veto over NHS vaccination teams
LSHTM finds dozens of schools block access and data sharing, herd immunity turns into logistics and incentives
Images
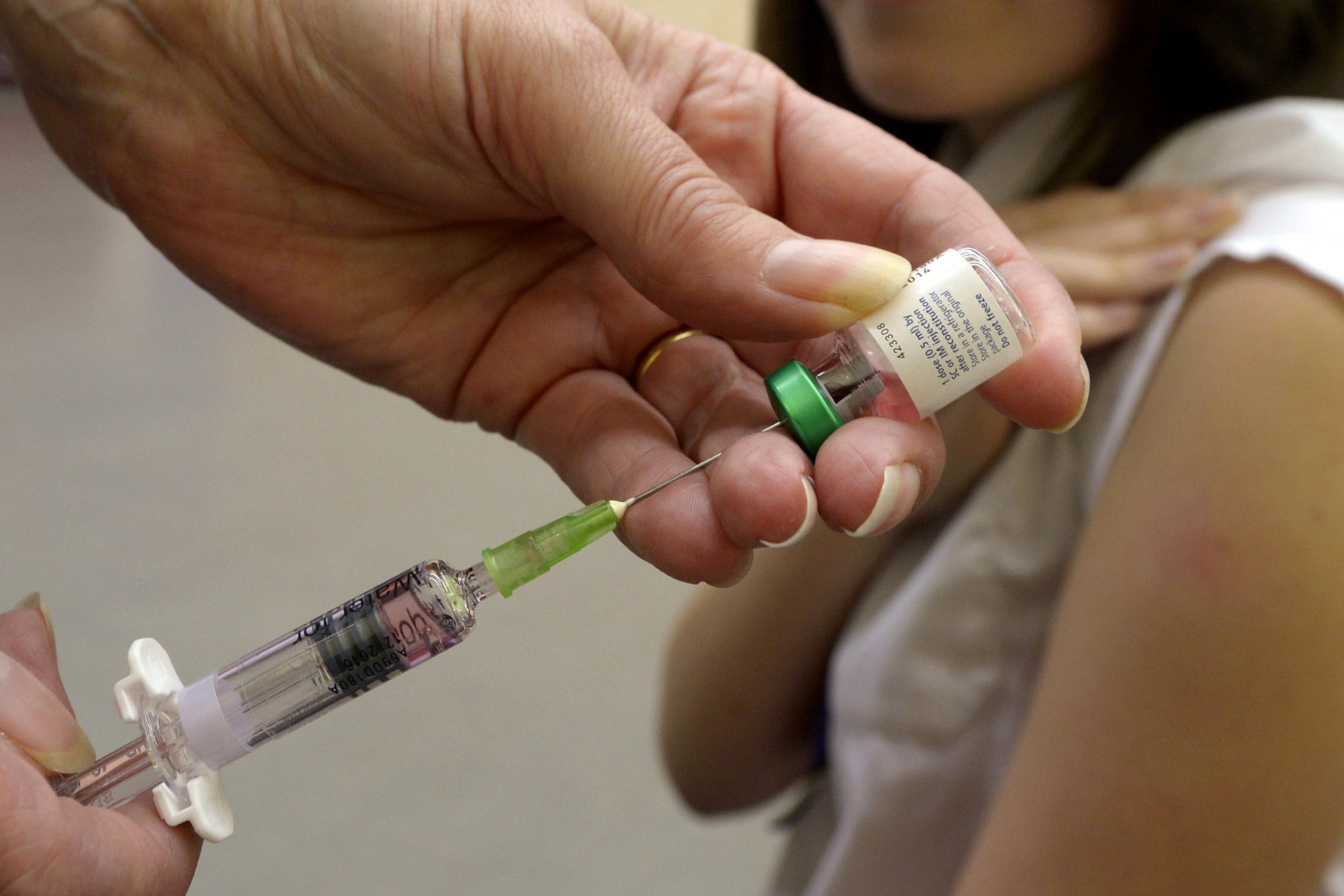 Take-up of both doses of the MMR vaccine is lowest in areas of London (PA)
independent.co.uk
Take-up of both doses of the MMR vaccine is lowest in areas of London (PA)
independent.co.uk
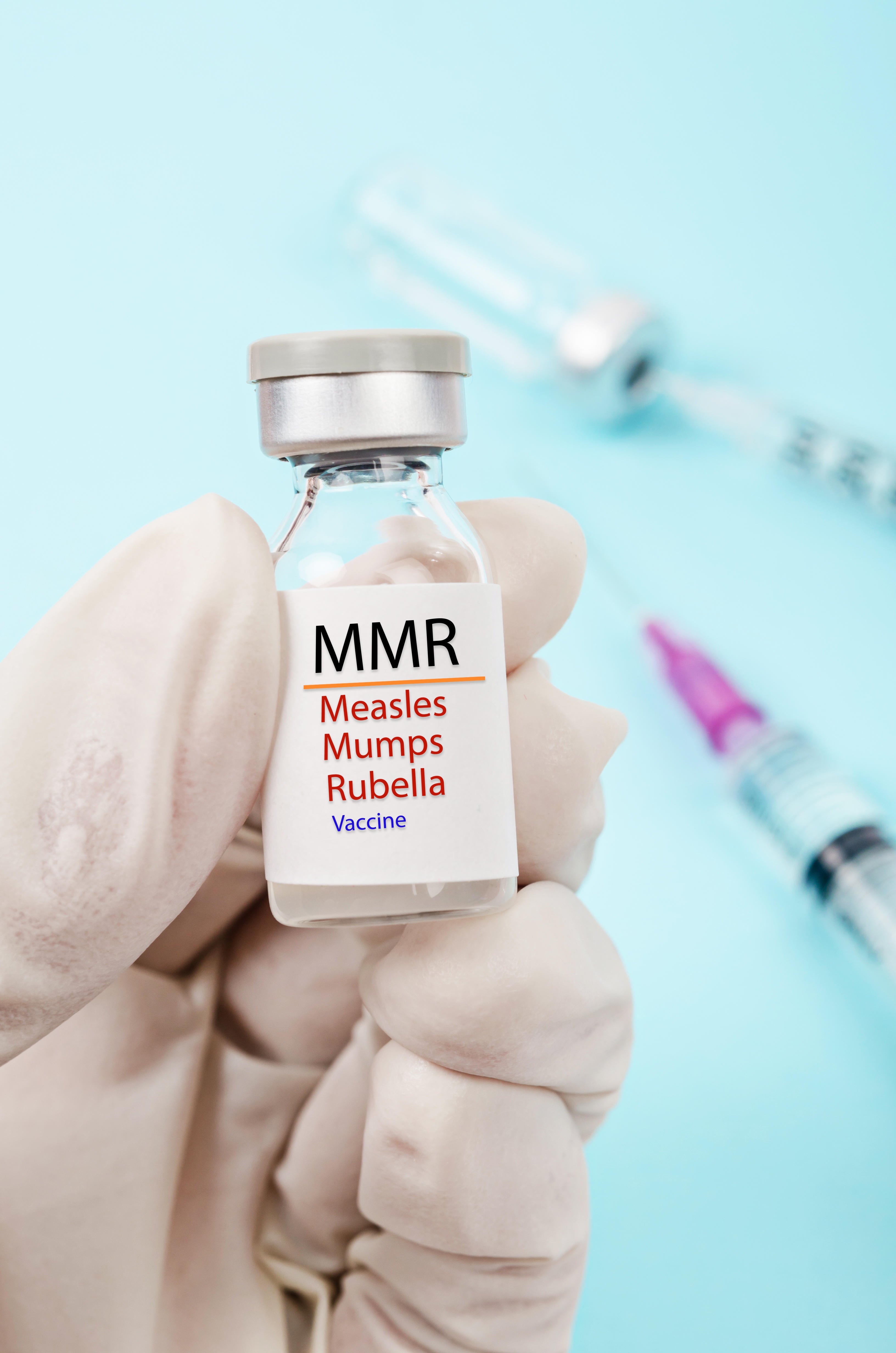 Two doses of the MMR are recommended to successfully protect against the virus (Alamy/PA)
Alamy/PA
Two doses of the MMR are recommended to successfully protect against the virus (Alamy/PA)
Alamy/PA
 The spots of the measles rash, which are not usually itchy, are sometimes raised and join together to form blotchy patches (Alamy/PA)
Alamy/PA
The spots of the measles rash, which are not usually itchy, are sometimes raised and join together to form blotchy patches (Alamy/PA)
Alamy/PA
A measles outbreak in Enfield, north London, has exposed a less-discussed bottleneck in “herd immunity”: access. According to The Independent, more than 50 suspected cases were reported by seven schools and a nursery, and dozens of schools in nearby boroughs have previously refused entry to NHS vaccination teams.
The key epidemiological point is not mysterious virology but network topology. Measles has a high basic reproduction number (R0), but in practice transmission is shaped by where susceptible people are concentrated. Schools are ideal amplifiers: dense contact rates, repeated exposure, and predictable mixing. When immunization coverage falls unevenly, you don’t get a smooth decline in population immunity—you get “susceptibility islands” that behave like dry tinder.
The Independent cites a London School of Hygiene and Tropical Medicine (LSHTM) study (published January 2026) finding that 32 of 450 schools in north east London (including parts of Hackney and Barking) “did not allow access” to school-age immunisation services, while at least 15 schools did not share information on which children needed catch-up shots. That is a logistics problem disguised as a public-health slogan.
UK Health Security Agency data show MMR two-dose coverage in 2024–25 at 65% in Haringey and 58.3% in Hackney, far below the oft-cited 95% target. In a school setting, that shortfall is not marginal; it changes the outbreak dynamics. With roughly one-third of children unprotected in some areas, contact tracing becomes triage: you can map chains, but you cannot “out-investigate” the arithmetic of too many susceptibles in high-contact nodes.
WHO figures for 2024–25, also cited by The Independent, underline the dose-response reality: over 1,000 unvaccinated children aged 5–15 contracted measles, compared with 183 with one dose and 123 fully vaccinated. That still leaves a politically inconvenient detail: breakthrough infections happen. University of Reading virologist Ian Jones told The Independent he was surprised to see cases among the double-vaccinated, noting timing and exposure intensity can matter.
Schools can act as veto points. LSHTM researchers warned the Department for Education in 2024 and called for rules requiring access for vaccination teams; former education minister Gillian Keegan replied, but it is unclear whether anything changed. The state promises herd immunity, then delegates the gatekeeping to institutions whose incentives include “not disrupting the school day.”
If Enfield spreads, it will not be because Britain forgot what measles is. It will be because a high-R0 virus found a set of human-made chokepoints—administrative, legal, and cultural—perfectly designed to keep needles out of the one place they matter most: clustered susceptibles.
