Epstein–Barr virus infects >95% for life
Latent B-cell reservoir links to cancers and multiple sclerosis, Near-universality makes biomarkers and co-factors the real battleground
Images
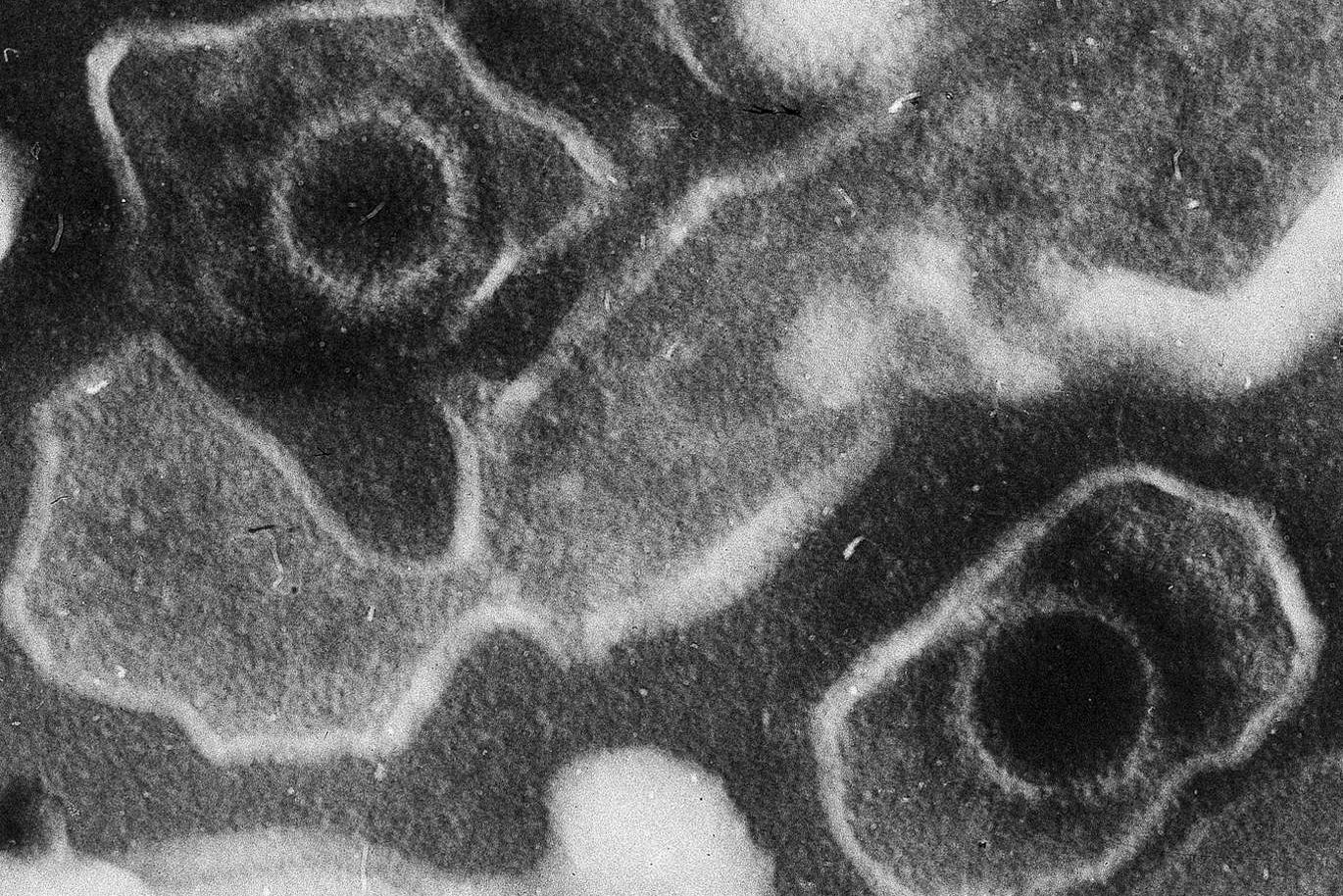 Epstein–Barr virus (EBV) (Liza Gross/CC BY 2.5)
Liza Gross/CC BY 2.5
Epstein–Barr virus (EBV) (Liza Gross/CC BY 2.5)
Liza Gross/CC BY 2.5
Epstein–Barr virus (EBV) is the closest thing modern medicine has to a universal infection: more than 95% of adults carry it for life, The Independent notes, usually without noticing. That near-ubiquity is not trivia; it is the baseline against which any claim about EBV “causing” disease must be judged. If almost everyone has it, then the scientific question is never simply presence/absence, but which measurable markers of infection and immune control actually predict later pathology.
EBV is a herpesvirus that establishes lifelong latency primarily in B cells. After primary infection—often asymptomatic in childhood, or manifesting as infectious mononucleosis when delayed into adolescence—it persists in a small pool of memory B cells. Reactivation can occur, typically under immune stress, but in immunocompetent hosts it is usually contained. This is why “reactivation” is a popular wellness bogeyman: it is real biology, but rarely a clinical event in itself.
Where the evidence hardens is in oncology and autoimmunity. EBV was the first virus demonstrated to contribute to certain cancers and is classified as a Group 1 carcinogen, according to the Independent’s summary. Mechanistically, EBV’s latent gene programs can drive B‑cell proliferation and survival; when immune surveillance fails—classically in immunosuppression—EBV-positive lymphoproliferative disease and EBV-associated lymphomas become more likely.
Multiple sclerosis (MS) is a frontier that tempts public health planners with the idea of a single microbial “lever” for a complex disease. The Independent, republishing a The Conversation piece by University of Limerick researcher Eanna Fennell, describes experimental work using mice with human-like immune systems: after EBV infection, B cells become unusually activated, migrate into the brain, and recruit T cells, producing inflammation and early tissue injury resembling hypothesized early MS processes. Depleting B cells with a commonly used therapy reduced T-cell infiltration and immune activation.
That fits with human observations that MS risk correlates with EBV history, and with the clinical reality that B‑cell–targeting therapies can be effective in MS. But it does not magically resolve the core epidemiological puzzle: if EBV is nearly universal, why isn’t MS? The Independent lists known co-factors—genetics, sex, smoking, obesity, and low vitamin D—implying that EBV may be necessary in many cases but insufficient on its own.
So what is actually predictive? Researchers look at serology (antibody titers to EBV antigens), evidence of recent reactivation (e.g., certain antibody patterns), and measures of immune competence. Viral load in blood is more useful in immunocompromised contexts than in the general population. The uncomfortable but honest answer is that no single, cheap EBV biomarker currently offers deterministic prediction for MS or cancer in the average carrier—because the signal is mostly in host response, not mere carriage.
If policymakers ever propose population-level EBV interventions, they should start by stating the obvious: when 95% of people are positive, “screen-and-act” becomes a mass program by default. That’s less a medical plan than an institutional appetite test.
